Two chairs. A piece of tape. And three cognitive interventions running simultaneously.
You've seen this patient.
They can follow instructions in a quiet room.
They can move their arm when you cue them.
They can answer your questions.
....But the moment you ask them to sit unsupported and reach at the same time....
👉 everything falls apart.
That's not weakness.
👉 That's cognitive load.
And this activity addresses all of it with two chairs, a piece of tape, three targets.
This is the fourth activity in this series built from materials that cost nothing. Two chairs exist in every clinic, every home, every waiting room. The tape you already have. The cognitive intervention is in how you set it up.
What the activity actually is
Setup:
🪑🪑 Two chairs facing each other
➿ A piece of tape or paper on the back chair as a target surface
Three tiers: one target below midline, one at neutral, one above shoulder height — Patient seated on the front chair, hands in hand-under-hand position on the back chair
The task: patient reaches forward and down to the bottom target, returns to midline, reaches to the middle target, returns, reaches to the top target, returns.
That is one sequence.
Grading Ideas
👉 Grade by pushing the front chair forward — more distance means more trunk load.
👉 Grade by moving from supported sit to unsupported sit.
👉 Grade by adding trunk rotation — place targets in a corner so the patient must rotate to reach both sides.
👉 Grade by adding weight to the bar for progressive resistance.
Three tiers. Infinite progressions.
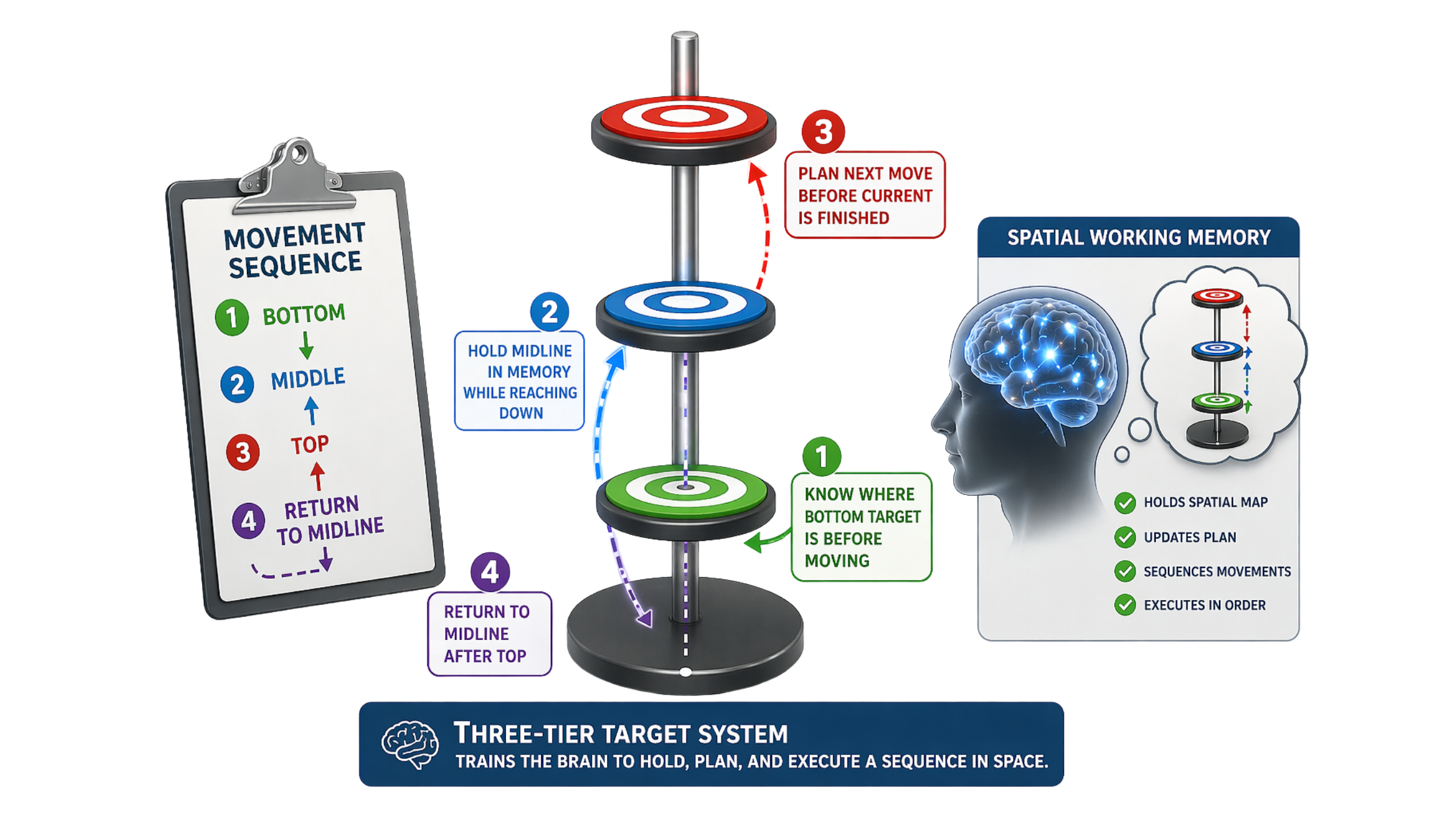
Why this is a spatial working memory intervention
Before the patient reaches to the bottom target —
👉 their brain has to know where the bottom target is.
Before they return to midline —
👉 their brain has to hold the midline location in working memory while executing the downward reach.
Before they move to the middle tier —
👉 their brain has to plan the next movement before the current one is finished.
That is anticipatory motor planning.
The three-tier target system forces the brain to hold a spatial map of the movement sequence — bottom, middle, top, return — and execute each element in order without losing the plan.
This is spatial working memory.
The same cognitive process that allows your patient to navigate their kitchen without bumping into things. To plan a transfer before they stand. To reach for an object on a shelf without knocking over what's next to it.
👉 The three targets are not just reach destinations.
👉 They are a spatial working memory protocol embedded in a seated activity.
When the patient loses their place in the sequence — reaches to the wrong tier, skips a target, needs repeated verbal cuing — that is not inattention.
👉 That is spatial working memory failure.
Document it as such.
Why this is a postural cognitive load intervention
Supported sitting is baseline.
The moment you remove the support — push the chair back, take away bilateral upper extremity weight-bearing — you have added a postural cognitive demand to every single movement.
Now the patient is simultaneously:
— Maintaining trunk alignment without support
— Planning and executing the reach sequence
— Holding the spatial map of the three tiers
— Monitoring the affected upper extremity through the unaffected hand
👉 That is a full dual-task postural-cognitive intervention.
The dual tasking cost framework applies here directly. If the patient's reach accuracy deteriorates when bilateral UE support is removed — if they start losing their place in the sequence, skipping tiers, or reaching off-target — you have identified the postural cognitive load ceiling.
👉 That is a functional safety finding.
A patient who cannot maintain spatial working memory for a three-tier reach sequence under postural demand is a patient who is at risk during any real-world activity that requires simultaneous trunk control and motor planning — transfers, bed mobility, reaching in the kitchen, getting dressed.
Document the ceiling. Grade to it systematically. That is skilled clinical reasoning.
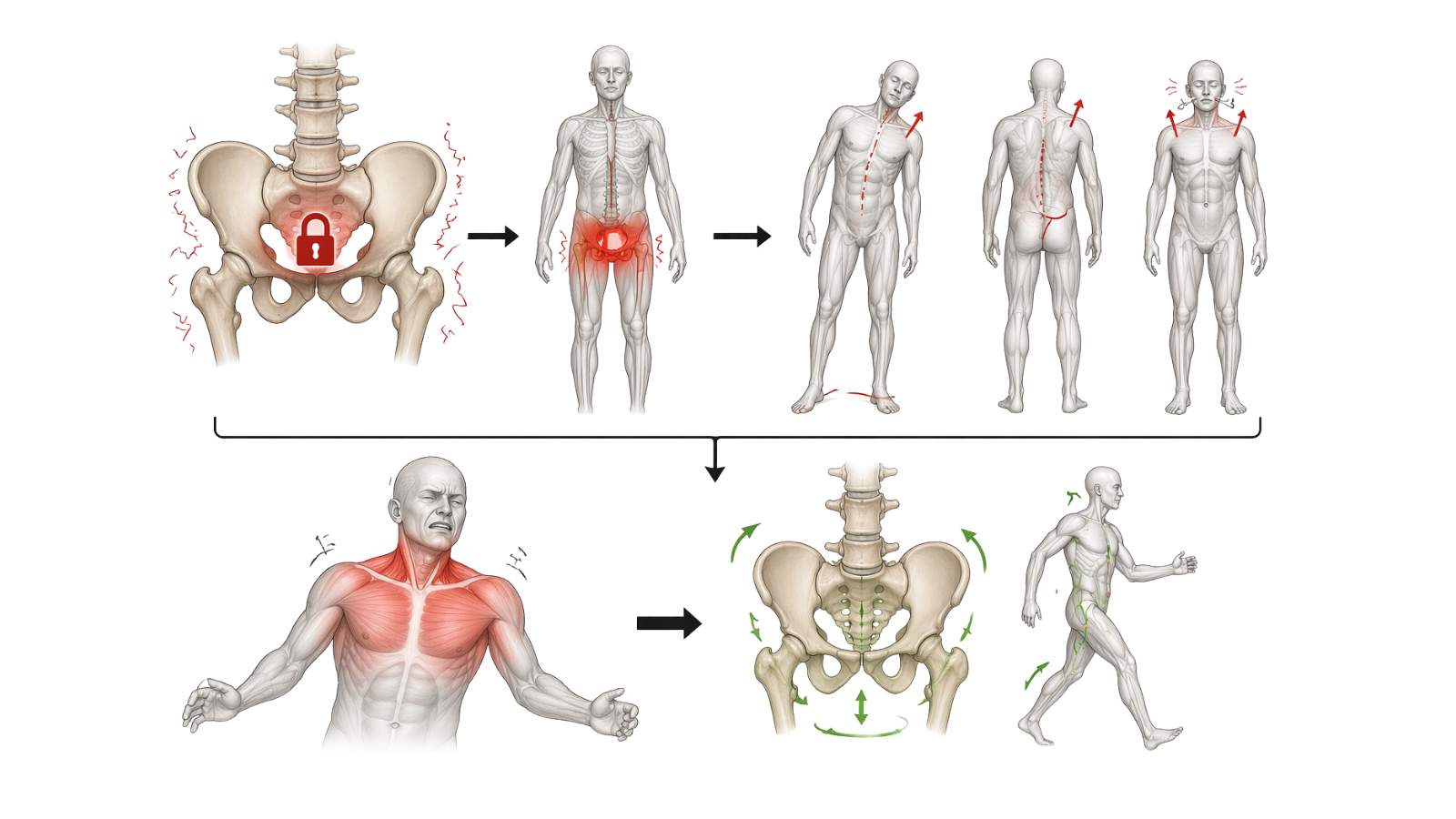
Why this is a motor initiation intervention
The pelvis is stuck.
👉 This is one of the most common and undertreated findings in neurological rehab.
Whether the cause is hemiplegia, chronic pain, deconditioning, or prolonged bed rest — a pelvis that cannot move freely is a pelvis that cannot support dynamic trunk movement superimposed on it. The patient compensates with their upper body. They hike their shoulder. They lean to one side. They hold their breath.
👉 None of that is a strength problem.
👉 All of that is a motor initiation problem.
The forward reach in this activity (especially when the chair is pushed forward to increase the load) forces pelvic anterior tilt and trunk flexion.
The return to midline requires the pelvis to actively participate in the movement rather than remain passive.
When you cue the patient to visualize their scapulas folding around their ribcage and their pelvis tilting forward, you are asking the brain to generate a motor command it has stopped generating automatically.
That is motor initiation.
The same executive function process that allows your patient to initiate getting out of bed in the morning, stand up from a chair without five verbal cues, or begin a task without being repeatedly prompted.
When the pelvis begins to move (when you see that forward tilt, that trunk flexion, that scapular protraction) that is not just mobility.
👉 That is the executive function system re-engaging with the motor system.
Document it as a skilled clinical outcome.