Small tools. Sophisticated neuroscience.
Somebody is going to look at this activity and think you're joking.
Let them.
That's it.
👉 That's the activity.
And yes — you can bill a 45-minute session on it.
Not because it looks impressive.
👉 Because what it's asking the brain to do is.
One note before we get into it: this is the third activity in a row built from materials that cost less than $10 combined. That's not a coincidence. The generalization argument holds here too — your patient has coins. They have binder clips. The motor map transfers.
What the activity actually is
Setup:
- A handful of coins
- Binder clips (various sizes — this is your grading tool)
- A receptacle: a cup, a box, a bowl — placed anywhere in the space
The task: patient picks up a coin using their target pinch pattern, picks up a binder clip, connects them into a two-part unit, and deposits the completed unit into the receptacle.
That's one unit. Two parts.
👉 Start with 5.
👉 Long-term goal: 25 units without tremor, fatigue, or compensatory movement.
The patient sets the number. You give them the framework. They fill it in.
👉 That's self-efficacy built into the objective measure.
Why this is a cognitive flexibility intervention
This is the cognitive hook most clinicians miss.
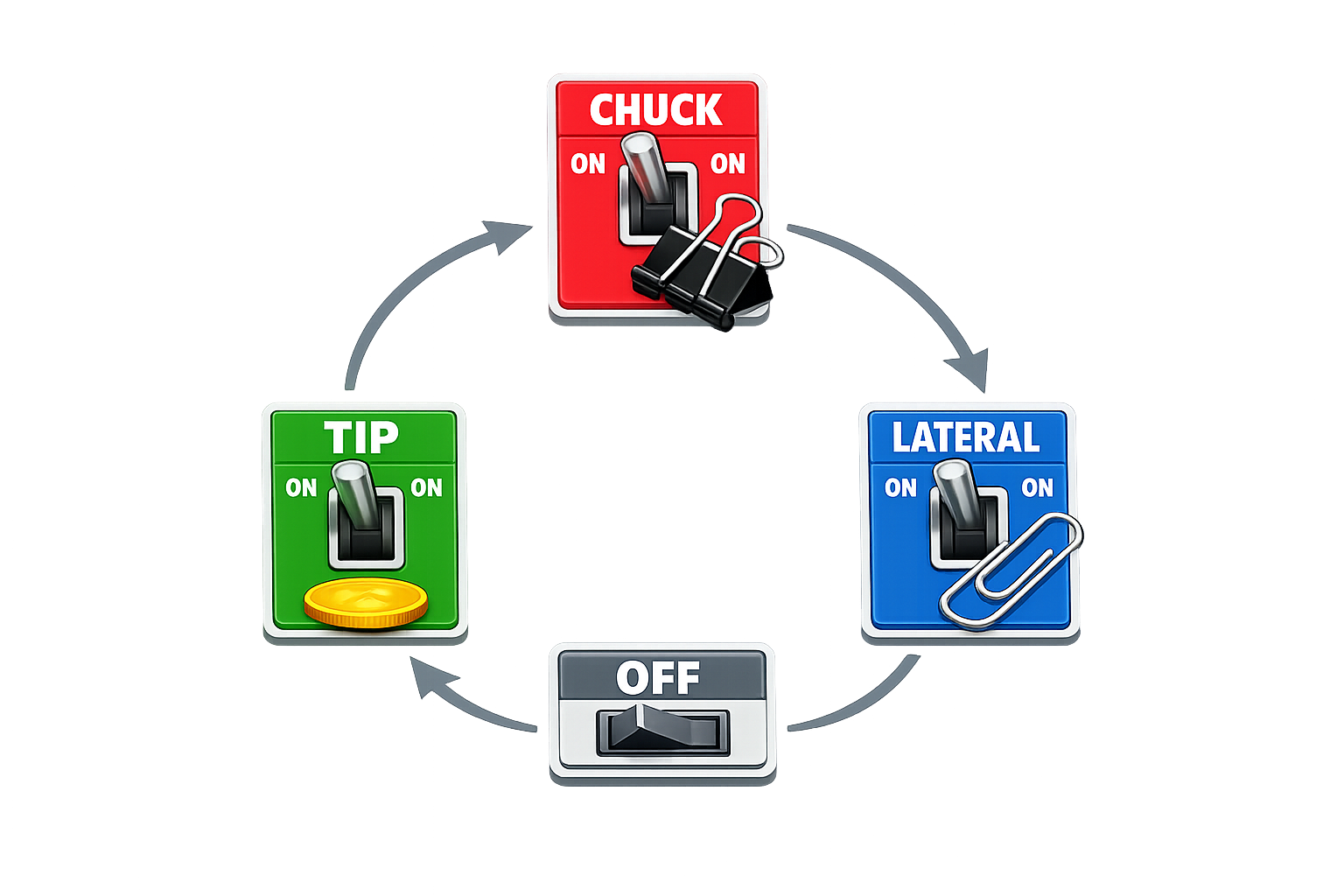
The activity is not just about pinch strength.
👉 It's about switching.
Tip pinch to pick up the coin. Chuck pinch to grip the binder clip. Lateral pinch to manipulate it open. Back to tip pinch to place it.
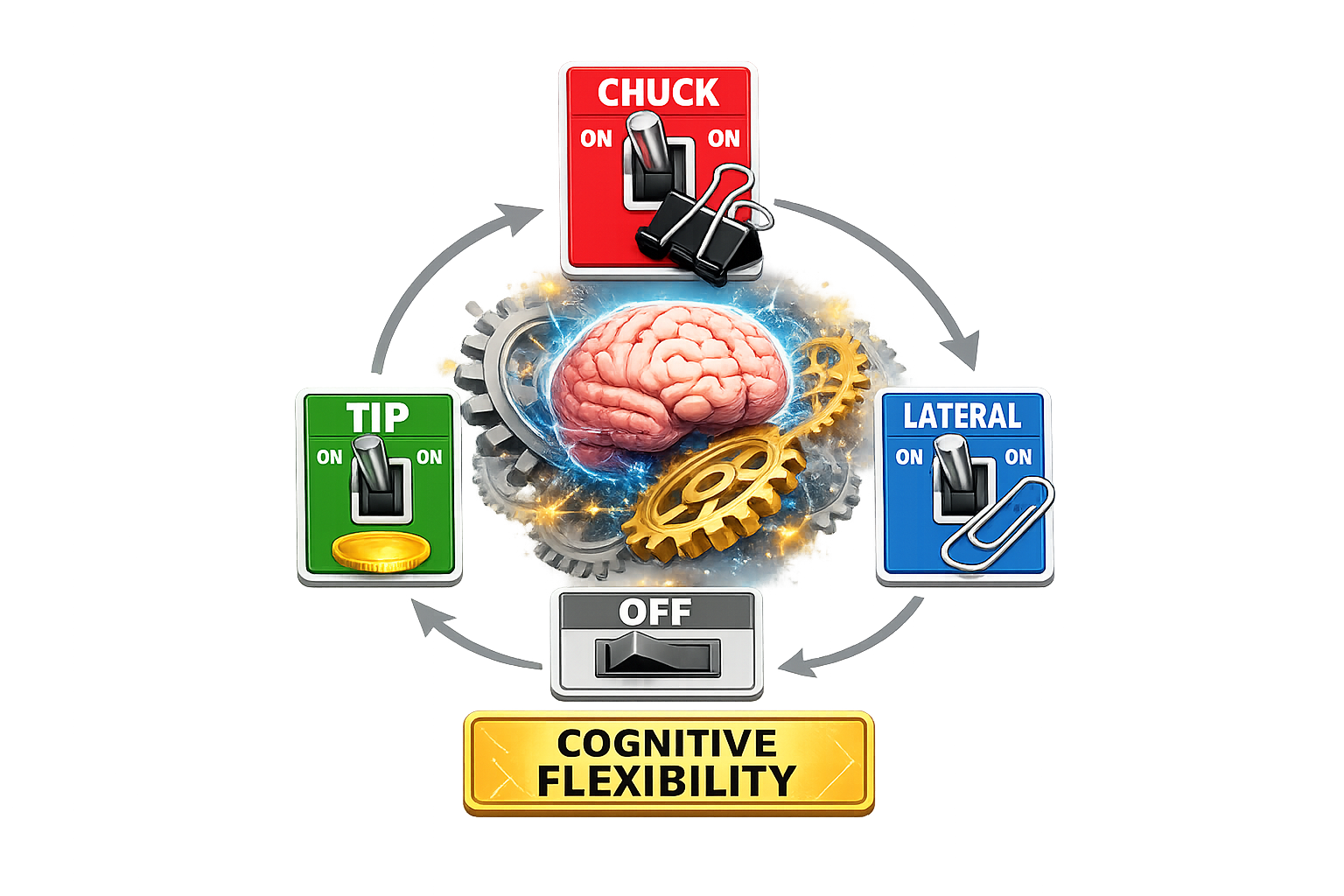
Every transition between pinch patterns requires the brain to:
— disengage the current motor program
— update the movement plan
— recruit a different set of intrinsic and extrinsic muscles
— execute the new pattern with control
👉 That is cognitive flexibility.
The same executive function that allows your patient to switch between tasks at home, change their plan when something unexpected happens, or adapt their movement when the context changes.

When cognitive flexibility breaks down:
— patients get stuck in one grip pattern regardless of the object
— they cannot update their motor plan mid-task
— they compensate with the whole hand instead of the right fingers
👉 That's not a strength problem.
👉 That's a motor planning and cognitive flexibility problem.
And binder clips — because they require a specific sequence of grip, compress, and release — are one of the most efficient ways to train it.
Why this is a spatial planning intervention
Where you put the receptacle is a clinical decision.
👉 Not a setup preference.
Receptacle directly in front: baseline reaching in the sagittal plane.
Receptacle to the affected side: crossing midline, visual scanning toward the neglected field.
Receptacle behind the patient: trunk rotation required to reach and deposit — full axial movement integrated into the task.
Receptacle on the floor: trunk flexion, forward reach, postural challenge.
[Modify standing suface + receptacle] Patient on a balance disc : postural control under concurrent fine motor demand.
👉 Each one is a different spatial working memory and motor planning demand.
👉 Each one requires the brain to plan the movement trajectory before executing it.
That is anticipatory motor planning — prefrontal executive function embedded in a coin and a binder clip.