The Cashier Who Can't Make Change
Your patient works as a cashier. Or they did, before the stroke.
Making change. Counting coins out of a drawer into a palm. Holding the handful while the other hand processes the receipt. Sliding the right coin forward with the thumb while the rest stay cupped in the palm.
👉 That is tip pinch, palm-to-finger translation, sustained hypothenar activation, and working memory — in a fifteen-second interaction at a register.
And it's gone.
Not because the hand is weak. Not because the patient isn't trying. Because the neuromuscular communication pathway from the brain to the small intrinsic muscles of the palm has been disrupted — and nobody has built it back yet because nobody has measured it precisely enough to know exactly where it broke.
This activity measures it. All of it. At once.
Fifteen beads. Five colors. PVC pipe connectors as receptacles. A timer and a tracking sheet. That is the entire setup — and it gives you endurance data, in-hand manipulation data, and working memory data in a single four-minute baseline that you can replicate at every session and track across your entire plan of care.
This is not a bead activity.
👉 This is a neuromuscular communication assessment dressed up as a bead activity.
And before the first bead leaves that palm, your patient needs to know the difference.
What the activity actually is
The tools:
🔵 15 small beads — five each of three colors, or three each of five colors
🔩 PVC pipe connectors used as receptacles — one per color, arranged on the tabletop in a consistent position before the session starts
⏱️ A timer
📋 A tracking sheet: time to complete, number of drops, number of errors, color sequencing accuracy
The setup:
Patient seated at the table with good postural alignment. All 15 beads placed into the patient's palm at once — not handed one at a time, not selected from a pile. Into the palm. Hand closes. That moment of closure is already data.
Receptacles are arranged by color directly in front of the patient, visible and within reach, not moved again until the session ends.
The task:
Patient inches each bead from palm to tip pinch, one at a time, and releases it into the correct color receptacle — while keeping the remaining beads cupped in the palm throughout.
That is one sequence. Fifteen repetitions. Every bead is a data point.
Before the first bead moves — lead with science every time
The thirty seconds before the activity begins are not setup time. They are your first clinical intervention.
If your patient thinks they are sorting beads into containers, they are sorting beads into containers. If your patient knows they are retraining the neuromuscular communication pathway between their prefrontal cortex and the intrinsic muscles of their palm — that the brain's ability to send precise, sustained signals to the small muscles that keep the hand cupped has been disrupted, and that every translation cycle in this activity is a repetition of that signal — they are doing something with a functional destination.
Name that destination before the first repetition. Every session.
"You told me it's hard to manage change at the register. What's happening is that your brain isn't sending a strong enough signal to the small muscles in your palm to keep your hand cupped while your fingers are working at the same time. That's what we're addressing right now. Every time you inch a bead up to your fingertips without dropping the ones behind it, you are retraining that signal."
👉 That is not motivation. That is encoding. The brain learns faster when the movement has meaning attached before practice begins. This is a non-negotiable part of the protocol — not a preamble to skip when the session is running long.
Patients who understand the science do not feel like they are doing kindergarten work. Patients who do not understand the science sometimes do. The science is your protection — for the therapeutic relationship and for the motor learning itself.
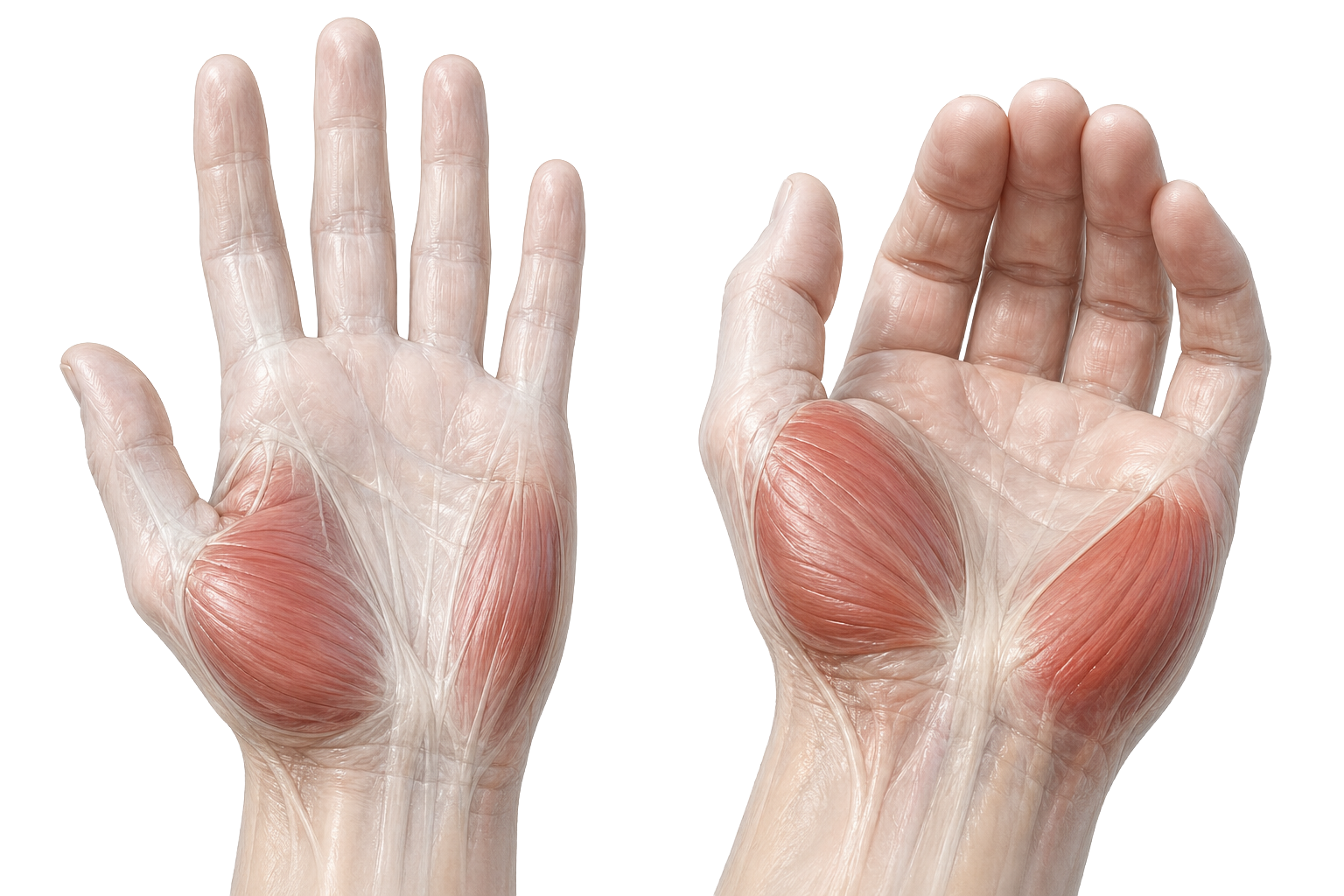
Why this is a sustained grasp endurance intervention
Fifteen beads in the palm. Hand closed. Pinky engaged.
👉 Watch the pinky.
The fingers doing the translation will look busy and purposeful. They are moving, they are doing something visible. The pinky is where the session actually is.
The moment the pinky begins to extend at the MCP joint, you have your finding. The hypothenar eminence is fatiguing under load. The ulnar cup is collapsing. The beads that were being contained in the palm by that ulnar border are now at risk — and your patient is about to drop one, compensate by gripping tighter with the remaining fingers, or shift into a pattern that protects the remaining beads at the cost of the translation quality.
All three of those responses are different clinical findings. Watch for which one your patient defaults to.
The thenar and hypothenar eminences together are what drive the palm's ability to cup and sustain a cup while the fingers are simultaneously active. This is not grip strength in the conventional sense. It is sustained intrinsic activation under concurrent motor demand — the palm holding while the fingers are working, both at the same time, neither able to rest while the other operates.
👉 The functional equivalent of this is every task that requires a patient to hold something in their palm while their fingers are doing something else simultaneously.
Making change. Holding crackers while a child eats from your palm. Carrying a handful of pills to the bathroom without dropping them. Managing keys while unlocking a door. Holding a cloth while wiping a surface. Every one of these tasks requires the same split — palm sustaining, fingers translating — and every one of them is inaccessible to a patient whose hypothenar eminence cannot stay engaged past the first thirty seconds of load.
Note which bead number triggered the pinky extension. Note whether it was gradual drift or a sudden drop. Note whether the patient noticed it or whether it was invisible to them. That bead number is your sustained endurance threshold. It is your baseline. That is the number you are moving across your plan of care — and it is objective, replicable, and directly functionally meaningful.
Why this is an in-hand manipulation intervention
The movement from palm to tip pinch is not a reach. It is a translation — and it is one of the most functionally demanding fine motor operations the hand performs.
The patient is not picking the bead up off a surface. They are moving it from a position inside the palm, held in place by the intrinsic muscles, upward through the digit pads to a tip pinch position at the fingertips — without using the other hand, without using a surface to assist, and without dropping the beads still remaining in the palm behind it.
Each bead is a full translation cycle:
— Intrinsic muscles shift the bead from the palm toward the distal digits — Digits receive it and position it for tip pinch — Tip pinch achieves the precision grip needed to release the bead accurately into the correct receptacle — Palm re-closes. Remaining beads are re-contained. The cycle begins again.
👉 Fifteen beads is fifteen full translation cycles without a break in the sustained grasp between them.
What you are watching across those fifteen cycles is the degradation curve. Where does tip pinch begin to lose precision? Where does the patient start compensating with lateral pinch instead — sliding the bead to the side of the index finger rather than lifting it cleanly to the fingertips? Where does the translation slow down, or speed up at the cost of accuracy? Where does the release become inaccurate — dropped short of the receptacle, released too early, or pushed in rather than placed?
Each of these degradation patterns points to a different underlying impairment. A patient who maintains tip pinch accuracy but slows progressively has a motor endurance profile. A patient who maintains speed but shifts to lateral pinch compensation has a motor planning or intrinsic weakness profile. A patient who loses accuracy in the final five beads regardless of pattern has a fatigue-sensitive fine motor coordination ceiling.
👉 Document which pattern you observed. They are not interchangeable, and they do not respond to the same intervention.

Why this is a working memory intervention
Fifteen beads. Five colors. Five receptacles. A rule that must stay active for every single repetition.
Before the patient translates a bead to tip pinch —
👉 their brain has to identify the color while it is still in the palm.
Before they release it into a receptacle —
👉 their brain has to hold the color-to-location mapping while simultaneously executing the translation and the reach to the correct container.
Before the next bead cycle begins —
👉 their brain has to update the internal record of what has already been sorted — without losing the spatial map of which receptacle holds which color and without letting that cognitive monitoring disrupt the motor plan for the next translation.
That is working memory. Not incidentally — structurally. The color sorting rule is a held cognitive constraint that must remain continuously active across all fifteen repetitions while the motor task runs concurrently. This is the same cognitive architecture required for medication management, for meal preparation sequencing, for any multi-step functional task where the patient must hold a rule or a plan in mind while their hands are doing something else.
👉 When the patient places the wrong color in a receptacle — when they look uncertain mid-reach, pause, or glance back to check what they already sorted — that is not inattention.
👉 That is working memory failure under concurrent motor load.
Document it as such. Record how many errors occurred, at which bead number they appeared, and — critically — whether the patient self-detected the error or required external cuing to identify it. Self-detection is a different cognitive finding than error blindness. A patient who places incorrectly and immediately notices has intact error monitoring with a working memory encoding failure. A patient who places incorrectly and continues without noticing has an error monitoring deficit on top of the working memory load problem. Both belong in your note. Both point to different intervention targets.
The grading structure built into this task is precise and independent. To increase the working memory demand without changing the motor demand — keep the same beads, same connectors, same 15-bead load — and increase the color complexity, add a recall probe after the lids are closed, or ask the patient to retrieve a specific color by name without opening all containers. Each variation targets working memory independently. Never advance motor and cognitive complexity in the same session.